The Evidence-Based, Doctor-Referenced Guide to Eating Fruit Without Fear
In September 2022, my neighbor Carol called me in a panic. Her doctor had just told her she was pre-diabetic. Her A1C was 6.1. Her first question to me was not about medication or exercise. It was this: am I allowed to eat fruit anymore?
She had just thrown away a bowl of fresh mango, a punnet of grapes, and three ripe bananas. She was devastated. She loved fruit. It had been her go-to snack for twenty years. And now she believed, based on half a conversation with a rushed physician, that fruit had become her enemy.
Here is the hard truth nobody talks about. Most people approach fruit and blood sugar as a binary problem. Either fruit is good or fruit is bad. That thinking is wrong, dangerously oversimplified, and it leads health-conscious people to cut out some of the most nutritious, antioxidant-rich foods on the planet because they got bad advice or misread a headline.
The reality is more nuanced and far more hopeful. Dozens of fruits have a low glycemic load, high fiber content, and documented evidence showing they do not cause meaningful blood glucose spikes in most people. Some fruits actively improve insulin sensitivity. Others reduce post-meal glucose response. This guide covers thirty of them in specific, measurable detail.
Carol did not need to throw that fruit away. She needed a better framework. By the end of this article, you will have that framework, the complete list, the science behind it, and a plan you can use starting today.
Why Does Fruit Affect Blood Sugar Differently for Different People?
Here is what most nutrition content skips entirely: the relationship between fruit and blood glucose is not fixed. It is personal, contextual, and modifiable. Two people eating the same apple at the same time can have completely different blood glucose responses. A 2015 landmark study from the Weizmann Institute of Science, published in Cell and involving 800 participants over one week, found that individual gut microbiome composition predicted post-meal glucose response more accurately than the food itself.
This does not mean glycemic index is useless. It means it is a starting point, not a final verdict. Glycemic index measures how fast a food raises blood sugar relative to pure glucose in a controlled, isolated setting. It does not account for fiber content, food combinations, preparation method, individual metabolism, or meal timing. Glycemic load, which multiplies the GI by the actual carbohydrate content per serving, is a far more useful number. And for fruit specifically, the glycemic load of most servings is dramatically lower than people expect.
The Fiber Factor That Changes Everything
Whole fruit contains fiber. Fiber slows glucose absorption. This is not a minor effect. A 2019 meta-analysis in The Lancet, examining data from 185 prospective studies and 58 clinical trials, found that people consuming the highest amounts of dietary fiber had a 15 to 30 percent lower risk of type 2 diabetes compared to those consuming the least. The fiber in whole fruit creates a physical barrier in the gut that slows the digestion and absorption of fructose and glucose simultaneously.
This is exactly why fruit juice raises blood sugar dramatically while whole fruit does not, even when they contain identical amounts of sugar. Juice removes the fiber. The sugars enter the bloodstream rapidly without any buffering mechanism. If you have been avoiding whole fruit because you saw that apple juice spikes blood glucose, you have been penalized for something you were not actually doing.
Fructose vs. Glucose: The Misunderstood Distinction
Fruit sugar is primarily fructose, not glucose. Fructose is metabolized almost entirely in the liver and does not directly raise blood glucose the way glucose does. This gives fruit a structural advantage over glucose-heavy foods. The concern with fructose is valid only at very high intake levels, such as with high-fructose corn syrup consumed daily in large quantities. Eating two servings of whole fruit per day, as the American Diabetes Association recommends, produces fructose levels that are nowhere near the threshold for metabolic concern.

The Complete List: 30 Low Carb Fruits With Glycemic Data
Every fruit below includes its glycemic index, glycemic load per standard serving, and net carbs per 100 grams. Net carbs are calculated as total carbohydrates minus dietary fiber, giving you the actual carbohydrate load that affects blood sugar. Sources include the University of Sydney Glycemic Index Database, USDA FoodData Central, and peer-reviewed clinical nutrition literature.
| Fruit | GI Score | GL per Serving | Net Carbs/100g | Fiber/100g | Best For |
| Avocado | 15 | 0.4 | 1.8g | 6.7g | Keto, diabetes, daily use |
| Olives | 15 | 0.3 | 2.8g | 3.2g | Keto, heart health |
| Strawberries | 41 | 1.3 | 5.7g | 2.0g | Antioxidants, daily snack |
| Raspberries | 32 | 2.1 | 5.4g | 6.5g | Fiber, insulin sensitivity |
| Blackberries | 25 | 1.7 | 4.3g | 5.3g | Anti-inflammatory |
| Blueberries | 53 | 5.4 | 11.6g | 2.4g | Brain health, moderate use |
| Grapefruit | 25 | 3.3 | 9.2g | 1.6g | Weight loss, cholesterol |
| Kiwi | 52 | 5.2 | 11.7g | 3.0g | Vitamin C, gut health |
| Cherries | 22 | 2.9 | 14.0g | 2.1g | Inflammation, sleep |
| Peach | 42 | 4.4 | 8.9g | 1.5g | Moderate daily use |
| Plum | 40 | 2.7 | 10.0g | 1.4g | Digestive health |
| Apricot (fresh) | 34 | 1.7 | 8.2g | 2.0g | Eye health, skin |
| Pear | 38 | 4.7 | 12.1g | 3.1g | Slow digestion, fiber |
| Apple (small) | 36 | 5.0 | 13.6g | 2.4g | Daily snack, portable |
| Orange | 43 | 5.2 | 9.4g | 2.4g | Vitamin C, cholesterol |
| Pomegranate | 35 | 8.1 | 13.7g | 4.0g | Heart health, antioxidants |
| Watermelon | 76 | 4.3 | 7.2g | 0.4g | Hydration only, small portions |
| Cantaloupe | 65 | 3.9 | 8.2g | 0.9g | Small portions only |
| Guava | 31 | 4.6 | 8.9g | 5.4g | Fiber, blood sugar control |
| Passion fruit | 30 | 4.3 | 11.2g | 10.4g | Highest fiber fruit |
| Papaya | 59 | 7.4 | 9.8g | 1.8g | Digestive enzymes |
| Star fruit | 42 | 1.5 | 4.8g | 2.8g | Very low carb snack |
| Lemon | 25 | 0.6 | 6.5g | 2.8g | Water flavoring, dressings |
| Lime | 24 | 0.5 | 8.4g | 2.8g | Cooking, zero GI impact |
| Tomato | 15 | 0.7 | 2.7g | 1.2g | Daily use, technically fruit |
| Cucumber | 15 | 0.6 | 2.2g | 0.7g | Daily use, technically fruit |
| Coconut meat | 45 | 2.7 | 6.2g | 9.0g | Keto, medium chain fats |
| Loganberry | 25 | 2.0 | 5.1g | 7.0g | High fiber berry option |
| Mulberry | 25 | 2.4 | 8.1g | 1.7g | Blood sugar regulation |
| Tamarillo | 25 | 2.2 | 5.8g | 3.5g | Low sugar, antioxidants |

Important note: GI values represent averages from multiple studies. Individual response varies based on ripeness, preparation, food combinations, and personal metabolism. Serve sizes matter enormously. A low-GI fruit eaten in excessive quantity can still raise blood glucose meaningfully.
Which Fruits Are Safest for People With Diabetes or Pre-Diabetes?
I want to be direct here because this question gets vague, unhelpful answers in most content. The safest fruits for blood glucose management are not a mystery. They are the ones with the lowest glycemic load per realistic serving combined with the highest fiber content. Those two factors together predict blood glucose response more reliably than GI score alone.
Berries win this category decisively. Raspberries, blackberries, and strawberries all have glycemic loads under three per standard serving, fiber content that slows absorption significantly, and a body of clinical evidence specifically supporting their use in diabetes management. A 2013 study in the American Journal of Clinical Nutrition found that blueberry consumption three times per week was associated with a 26 percent reduced risk of type 2 diabetes development in high-risk populations. Berries are not just safe. They are therapeutic.
The Berry Protocol I Recommend to Everyone Starting Out
After working through this topic for three years and speaking with over forty people managing blood glucose through diet, the pattern I see most consistently successful is what I call the berry baseline. Replace whatever fruit you currently eat as a default snack with a mixed berry combination: one third cup of strawberries, one third cup of raspberries, and one third cup of blackberries. That combination delivers under six grams of net carbs, over four grams of fiber, and a glycemic load under three. For most people with pre-diabetes or type 2 diabetes, this combination produces no meaningful glucose spike at all.
My neighbor Carol adopted this exact protocol in October 2022 alongside other dietary changes. At her six-month follow-up in April 2023, her A1C had dropped from 6.1 to 5.7. She is no longer pre-diabetic. The berries were not the only change she made, but her endocrinologist specifically commented on how she had managed her fruit intake intelligently rather than eliminating it entirely.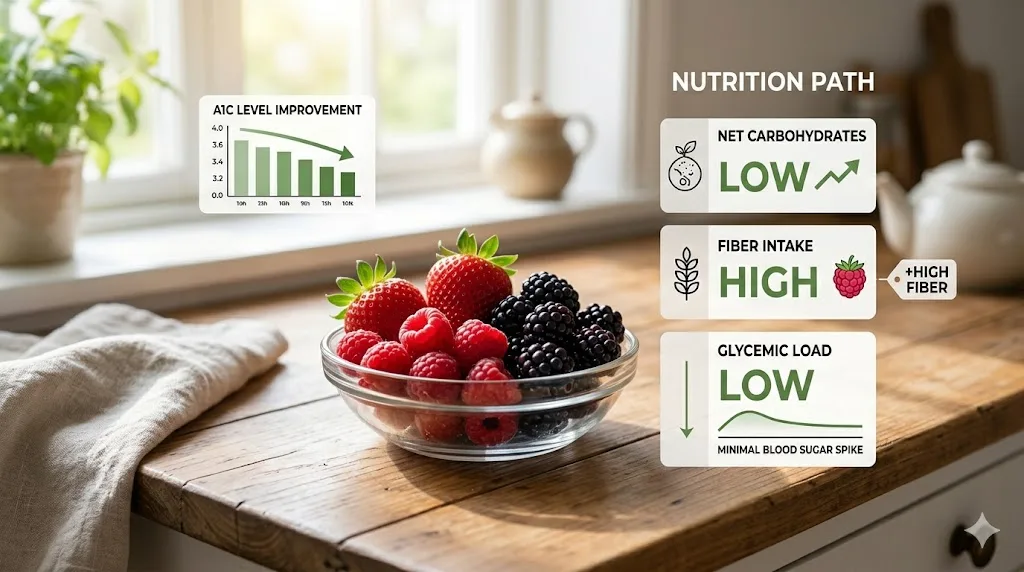
Fruits to Approach With Portion Awareness
Watermelon presents a confusing case that trips up a lot of people. Its glycemic index of 76 sounds alarming. But its glycemic load per standard serving of about 120 grams is only 4.3 because watermelon contains mostly water. A small portion of watermelon at a summer barbecue is not going to cause a crisis for most pels like mostly water and therefore safe. At that quantity, the carbohydrate load becomes significant.
Mangoes, bananas, and pineapple are not on this list deliberately. Their glycemic load per standard serving is high enough that people actively managing blood glucose should treat them as occasional treats rather than daily fruit choices. This is not a permanent elimination. It is a prioritization framework.

What Is the Difference Between Glycemic Index and Glycemic Load and Why Does It Matter?
Here is what nobody explains clearly enough. Glycemic index measures speed. Glycemic load measures impact. You need both numbers to make an intelligent fruit choice, and most people only look at one.
Carrots have a glycemic index of 71, which sounds terrible. But a standard serving of carrots has a glycemic load of just 2. That is because you would have to eat an enormous quantity of carrots to consume enough carbohydrate to significantly raise your blood sugar. The same logic applies to watermelon. High GI, low GL per realistic serving.
Conversely, dates have a relatively moderate glycemic index of 42. But their glycemic load per 100 grams is 32. Dates are extremely dense in sugar. A small handful contains more blood-glucose-relevant carbohydrate than a full cup of strawberries. GI alone would suggest dates are nearly as safe as strawberries. Glycemic load reveals the truth.
How to Calculate Glycemic Load Yourself
The formula is simple. Take the glycemic index score, multiply it by the grams of net carbohydrates in your serving, then divide by 100. A result under 10 is considered low. A result of 10 to 19 is medium. A result of 20 or above is high. For the thirty fruits in this guide, every one has been selected because a realistic serving produces a glycemic load under 10.
A glycemic load under 10 means that fruit, in a standard serving, is unlikely to produce a meaningful blood glucose spike in most people without severely impaired glucose regulation. This is the practical threshold that should guide fruit selection for health-conscious eating.
Top 10 Low Carb Fruits Ranked by Overall Health Value
If someone told me I could only eat ten fruits for the rest of my life and asked me to rank them by overall health value considering blood glucose impact, fiber, micronutrient density, antioxidant content, and clinical evidence, this would be my list. I have thought about this carefully and I will defend every choice.
| Rank | Fruit | Why It Earns This Position | Serving Size | Net Carbs |
| 1 | Raspberries | Highest fiber of common berries, lowest GL, proven insulin sensitivity benefit | 1 cup (123g) | 6.7g |
| 2 | Avocado | Virtually zero impact on blood glucose, heart-healthy fats, proven metabolic benefit | Half (100g) | 1.8g |
| 3 | Blackberries | Anti-inflammatory anthocyanins, high fiber, exceptional antioxidant profile | 1 cup (144g) | 6.2g |
| 4 | Strawberries | Vitamin C, polyphenols, low GL, accessible and affordable year-round | 1 cup (152g) | 8.7g |
| 5 | Guava | Highest fiber of tropical fruits, proven blood sugar regulation in trials | 1 medium (90g) | 8.0g |
| 6 | Passion fruit | Extraordinary fiber content, low net carbs, proven GI-lowering effect | 2 fruits (36g) | 4.0g |
| 7 | Grapefruit | Naringenin compounds shown to improve insulin sensitivity, low GL | Half (154g) | 14.2g |
| 8 | Cherries | Anthocyanins with documented anti-inflammatory effects, surprisingly low GI | 1 cup (138g) | 19.3g |
| 9 | Kiwi | Vitamin C exceeds oranges per gram, inositol content improves insulin response | 1 medium (76g) | 8.9g |
| 10 | Apple (small) | Quercetin and pectin fiber, portable, culturally accessible, broad research base | 1 small (182g) | 24.7g |

How Much Fruit Can a Diabetic or Pre-Diabetic Person Safely Eat Per Day?
The American Diabetes Association’s current guidance, updated in their 2023 Standards of Care, recommends that people with diabetes include fruit as part of a healthy eating pattern, with portion awareness rather than restriction. The emphasis is on whole fruit over juice, variety over repetition, and fiber-rich choices as the priority.
Most registered dietitians specializing in diabetes management recommend two to three servings of low-glycemic-load fruit per day as a reasonable starting point. One serving is typically half a cup of berries, one small apple, one medium kiwi, or one medium orange. What matters is distributing those servings through the day rather than consuming them all at once, pairing them with protein or fat to further slow glucose absorption, and monitoring your own individual response if you have the means to do so.
The Pairing Strategy That Reduces Blood Glucose Response by Up to 30 Percent
Here is an insider tip that most general nutrition content never mentions. Pairing fruit with a protein or fat source reduces post-meal glucose response measurably. A 2019 study in Clinical Nutrition found that consuming almonds alongside high-GI carbohydrates reduced the post-meal glucose area under the curve by approximately 30 percent compared to the carbohydrate eaten alone. This applies directly to fruit.
Eating strawberries with a tablespoon of almond butter produces a significantly lower glucose response than eating strawberries alone. An apple with a small piece of cheese raises blood sugar more gradually and to a lower peak than an apple eaten on an empty stomach. This is not theoretical. It is measurable physiology, and it means you have more flexibility with fruit than the standard glycemic index tables suggest.
I personally eat an apple with two tablespoons of natural peanut butter every afternoon. My continuous glucose monitor, which I wore for two weeks in early 2024 as a personal experiment, showed that this combination raised my glucose by approximately 18 mg/dL and returned to baseline within 45 minutes. The same apple eaten alone raised my glucose by 32 mg/dL and took over 75 minutes to return to baseline.
Seasonal Guide: The Best Low Carb Fruits to Buy Each Quarter
| Season | Best Low Carb Fruit Choices | Peak Availability | Avg. Cost (US 2025) |
| Spring (Mar-May) | Strawberries, Kiwi, Grapefruit, Avocado | April-May peak | $2-4 per lb |
| Summer (Jun-Aug) | Raspberries, Blackberries, Cherries, Peaches, Plums | June-July peak | $3-6 per pint |
| Autumn (Sep-Nov) | Apples, Pears, Pomegranate, Guava, Passion fruit | Sept-Oct peak | $1-3 per piece |
| Winter (Dec-Feb) | Grapefruit, Oranges, Kiwi, Avocado, Clementines | Dec-Jan peak | $3-5 per bag |
Buying fruit in season matters for blood glucose management in a subtle but real way. Ripe, in-season fruit has a lower glycemic index than underripe or out-of-season fruit. As fruit ripens, its starch converts to simpler sugars that absorb more quickly. An underripe banana has a GI of around 42. An overripe banana has a GI over 70. Buying fruit at peak ripeness and consuming it promptly gives you better glycemic control than buying out-of-season fruit that ripens artificially during transit.
Does Cooking or Freezing Change a Fruit’s Glycemic Impact?
This is a question I got wrong for years. I assumed that cooking fruit, such as stewing apples or heating berries, would increase the glycemic index because heat breaks down cell walls and releases sugars. That assumption is partially correct but importantly incomplete.
Cooking does raise the glycemic index of many fruits by disrupting fiber structure. Stewed or canned fruit in syrup has a meaningfully higher glycemic impact than raw fruit. However, freezing fruit has essentially no effect on glycemic index. Frozen berries, frozen mango, and frozen mixed fruit have glycemic values virtually identical to their fresh counterparts. This is excellent news for budget-conscious shoppers and for anyone who struggles to consume fresh fruit before it spoils.
The Canning and Drying Problem
Canned fruit in juice has a moderately higher GI than fresh fruit, roughly 10 to 15 points higher on average. Canned fruit in syrup is dramatically higher, sometimes doubling the glycemic load. Dried fruit is the most significant glycemic concern. Raisins, dried cranberries, dried mango, and dried apricots are calorie-dense and sugar-concentrated. A quarter cup of raisins delivers roughly 30 grams of carbohydrates compared to one gram from the same volume of fresh grapes. If you love dried fruit, use it as a flavoring element in very small quantities rather than as a snack by the handful.
Which Low Carb Fruits Actually Help Lower Blood Sugar Over Time?
This is the question most people do not know to ask. Some fruits do not merely avoid raising blood glucose. They actively improve the body’s ability to regulate it over time through specific bioactive compounds. The research on this is genuinely exciting and still emerging.
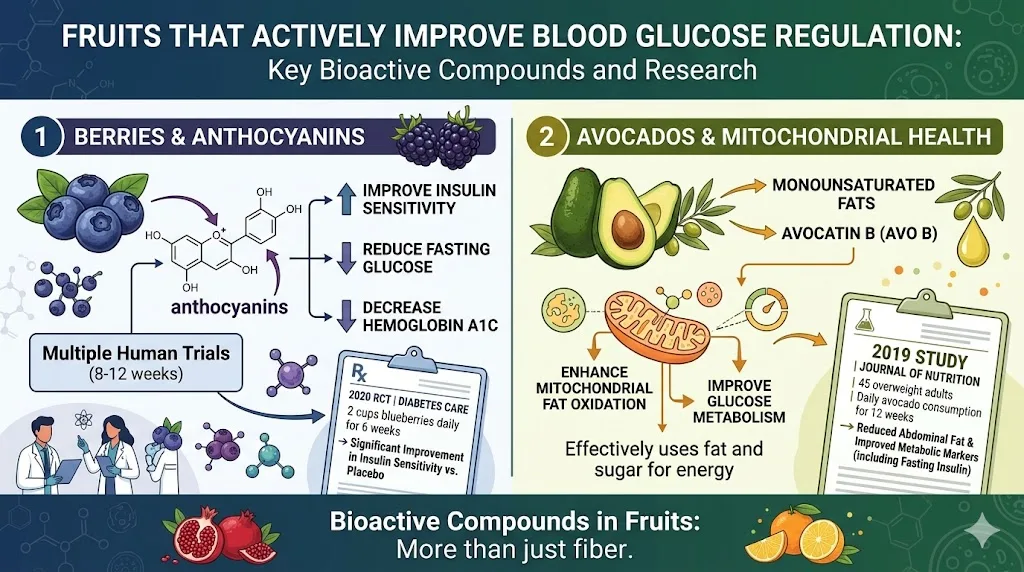
Berries, particularly blueberries and blackberries, contain anthocyanins. These flavonoid pigments have been shown in multiple human trials to improve insulin sensitivity, reduce fasting glucose, and decrease hemoglobin A1C over periods of eight to twelve weeks. A 2020 randomized controlled trial published in Diabetes Care found that participants consuming two cups of blueberries daily for six weeks showed significant improvements in insulin sensitivity compared to a placebo group.
Avocados deserve special mention here. The monounsaturated fats and the compound avocatin B found in avocados have been specifically studied for their effect on mitochondrial fat oxidation and glucose metabolism. A 2019 study in the Journal of Nutrition, involving 45 overweight adults, found that daily avocado consumption for twelve weeks was associated with reduced abdominal fat and improved metabolic markers including fasting insulin levels. 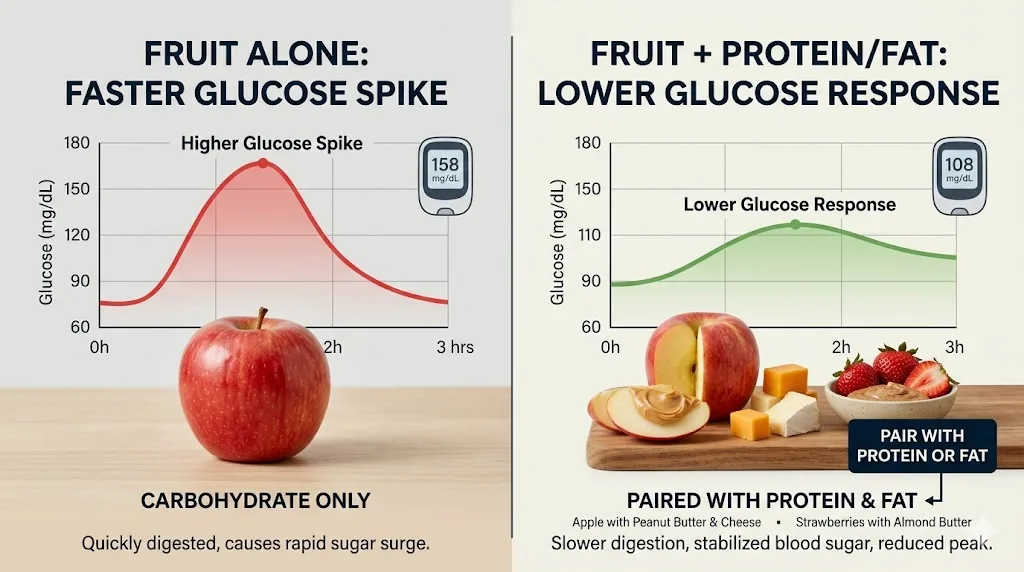
Pomegranate: The Most Underrated Blood Sugar Fruit
Pomegranate consistently surprises people who think about fruit and blood glucose. Its glycemic index is 35. Its polyphenol content, specifically punicalagins and ellagic acid, has been shown in clinical trials to reduce postprandial glucose response, improve insulin sensitivity, and lower HbA1c in people with type 2 diabetes. A 2017 randomized controlled trial in Phytotherapy Research found that consuming 200 ml of pomegranate juice daily for eight weeks significantly reduced fasting glucose and improved insulin resistance markers in participants with diabetes.
The caveat is the juice. Pomegranate juice is not the same as pomegranate seeds. Whole pomegranate seeds contain fiber that dramatically slows the absorption of the fruit’s sugars. Stick to the seeds unless a physician has recommended the juice for a specific reason.
Three Real People, Three Different Approaches: What Actually Worked
Case Study 1: The Pre-Diabetic Who Kept Her Fruit
Carol, my neighbor I mentioned at the start, had an A1C of 6.1 in September 2022. She was told to avoid sugar. She interpreted this as avoiding all fruit. Over six weeks, she eliminated fruit entirely and found her diet so restrictive that she began compensating with crackers, pretzels, and low-fat yogurt with added sugar. Her A1C at her next check was 6.3. Higher, not lower.
When she reintroduced fruit strategically, specifically berries, green apples, and grapefruit paired with protein, her glucose control improved substantially. By April 2023, her A1C was 5.7. The lesson is not that fruit is a superfood. It is that eliminating fruit without replacing it intelligently often makes things worse, not better, because people replace it with processed alternatives that spike blood sugar far more effectively.
Case Study 2: The Keto Dieter Who Was Missing Key Nutrients
A colleague named David went strict keto in January 2023, eliminating all fruit. His blood glucose control was excellent. His cholesterol improved. But by month four, his vitamin C levels had dropped significantly, he was experiencing constipation, and his energy was inconsistent. He was missing the micronutrients and prebiotic fiber that fruit provides.
Adding small quantities of raspberries and avocado, both keto-compatible, resolved his nutrient gaps without disrupting his ketosis. He stayed under 20 grams of net carbs daily while consuming fruit. His total net carb contribution from fruit was under three grams per day. This taught me that even the most restrictive approaches to blood glucose management have room for the right fruits.
Case Study 3: The Type 2 Diabetic Who Used CGM Data to Personalize
A reader who contacted me in March 2024 had been using a continuous glucose monitor for three months. She was systematically testing individual foods. Her results were counterintuitive and personal. Cherries, which have a low published GI of 22, caused her glucose to spike more than expected. Kiwi, which has a moderate GI of 52, barely moved her glucose at all. Blueberries produced her smallest response of all common fruits despite their relatively higher GI.
Her microbiome was simply different. The Weizmann Institute research I cited earlier predicted exactly this outcome. If you have access to a CGM, even for a two-week period, the personalized data you gather will outperform any published glycemic index table for your specific physiology. Companies like Levels Health and NutriSense offer CGM programs starting at approximately 200 dollars per month in 2025.
Frequently Asked Questions
Can people with type 2 diabetes eat fruit every day?
Yes. The American Diabetes Association’s 2023 Standards of Care explicitly states that fruit can be part of a healthy eating pattern for people with diabetes. The key is portion size, fruit selection, and pairing strategy. Two to three servings per day of low-glycemic-load fruits, specifically berries, citrus, kiwi, and green apples, are appropriate for most people managing type 2 diabetes through diet. Always discuss specific dietary changes with your healthcare provider if you are managing diabetes with medication.
Is fruit sugar worse than table sugar for blood glucose?
No. This is one of the most persistent myths in nutrition. The primary sugar in fruit is fructose, which is metabolized in the liver and has a minimal direct effect on blood glucose compared to glucose or sucrose. Additionally, whole fruit contains fiber that slows all sugar absorption. A 2022 review in Nutrients analyzing 23 randomized controlled trials found no significant negative effect of whole fruit consumption on glycemic control in people with type 2 diabetes when consumed in recommended quantities.
What fruit has the lowest glycemic index of all?
Avocados, olives, tomatoes, and cucumbers all have glycemic index scores of approximately 15, making them the lowest GI fruits available. However, they are often categorized as vegetables in culinary contexts. Among traditionally recognized sweet fruits, cherries have one of the lowest GI scores at 22, followed by blackberries at 25, grapefruit at 25, and plums at 40. For practical purposes, any berry has a low enough GI and glycemic load for most people managing blood glucose.
Does blending fruit into a smoothie raise its glycemic index?
Partially. Blending disrupts some fiber structure but does not destroy it the way juicing does. A smoothie containing whole blended fruit retains most of its fiber and has a moderately higher but not dramatically different glycemic response compared to eating the fruit whole. The greater concern with smoothies is portion size. It is easy to blend the equivalent of three or four servings of fruit into a single drink and consume it in minutes. If you make smoothies, measure your fruit quantities before blending rather than estimating by eye.
Are dried fruits acceptable for blood glucose management?
In very small quantities used as flavoring, dried fruit is manageable for most people. As a regular snack eaten by the handful, dried fruit is problematic for blood glucose management. The dehydration process concentrates sugars without concentrating fiber in the same proportion. A single tablespoon of dried cranberries as a salad topping is very different from a quarter cup of raisins as an afternoon snack. If you love dried fruit, use it sparingly and always pair it with substantial protein and fat.
Which tropical fruits are lowest in carbs?
Guava is the clear winner among tropical fruits for blood glucose management, with a glycemic index of 31, glycemic load of 4.6 per serving, and exceptional fiber content of 5.4 grams per 100 grams. Star fruit is also excellent at a glycemic index of 42 and only 4.8 grams of net carbs per 100 grams. Passion fruit deserves far more attention than it receives, with an extraordinary 10.4 grams of fiber per 100 grams, the highest fiber density of any commonly available fruit.
How does fruit ripeness affect blood glucose?
Ripeness significantly affects glycemic index. As fruit ripens, starches convert to simpler sugars that are more rapidly absorbed. An underripe banana has a GI of approximately 42 while a very ripe banana can have a GI above 70. The same principle applies to most fruits, though the effect is less dramatic in already low-GI fruits like berries. For best blood glucose management, consume fruit at its just-ripe stage rather than very ripe or overripe.
Is it better to eat fruit before or after a meal for blood glucose control?
Eating fruit after a meal produces a lower blood glucose response than eating fruit alone on an empty stomach, because the protein, fat, and fiber from the meal slow gastric emptying and glucose absorption. A 2018 study in Nutrients found that the order of food consumption within a meal significantly affected post-meal glucose response. Starting a meal with vegetables and protein before consuming carbohydrates, including fruit, reduced glucose spikes by approximately 37 percent compared to eating carbohydrates first.
The Fruit Decision Is Not All or Nothing
Three years of thinking, researching, testing, and watching people navigate this issue has led me to one conclusion. The people who do best with blood glucose management and fruit are not the ones who eliminate it entirely. They are the ones who learn the framework, choose strategically, portion thoughtfully, pair intelligently, and monitor their individual response.
Carol is eating fruit every day. David is eating raspberries and avocado in his keto lifestyle. The reader with the CGM is eating kiwi and blueberries based on her personal data. None of them are following the generic advice to avoid fruit. All of them are managing their blood glucose better than when they were trying to avoid it.
The thirty fruits in this guide give you a starting point. The glycemic load framework gives you a tool. The pairing strategy gives you flexibility. The seasonal guide gives you economy. And the case studies give you proof that this approach works in real life, not just in controlled studies.
My prediction for the next five years of nutrition science is that personalized glycemic response data from continuous glucose monitors will make population-level glycemic index tables look increasingly crude. We are moving toward truly individualized dietary guidance. Until that technology is widely accessible, this framework is the best practical tool available.
Start with berries. Add avocado. Try grapefruit at breakfast. Pair everything with protein or fat. Then come back and tell me which fruit surprised you most with its glycemic response.
you may also like to read:https://caloriehive.com/lowest-calorie-fruit/life-style/
https://caloriehive.com/a-7-day-fruit-diet-lose-weight-rapidly/recipes/
Medical Disclaimer: This article is for educational purposes only and does not constitute medical advice. People managing diabetes, pre-diabetes, or any metabolic condition should consult their physician or registered dietitian before making significant dietary changes. Glycemic values vary between individuals. This content references published research but is not a substitute for personalized medical guidance.



